A recent US study by the University of Colorado Boulder lets you measure the risk of airborne Coronavirus in our workplaces, schools and on public transport, National Geographic reports

Amid the pandemic, once normal activities are peppered with questions and concerns. Can kids go back to crowded schools? Is it safe to eat lunch with colleagues? Should we worry about going for a run?
A recent modeling effort may help provide some clues. Led by Jose-Luis Jimenez at the University of Colorado Boulder, the model estimates the riskiness of different activities based on one potential route of coronavirus spread: itty-bitty particles known as aerosols.
It is proven that COVID-19 can be spread through droplets. Coughing, singing, talking, or even breathing sends spittle flying in a range of sizes. The closer you are to the spewer, the greater the chance of exposure to large, virus-laden droplets that can be inhaled or land in your eyes.
But many scientists have also grown concerned about the potential risks of aerosols—the smallest of these particles—which may float across rooms and cause infections. It’s a worry that’s greatest where ventilation is poor and airborne particulates could build.
While more research is needed to conclusively demonstrate the role of aerosol transmission in the spread of the virus, the new model incorporates what is known about the coronavirus’s spread from case reports of potential airborne transmission.
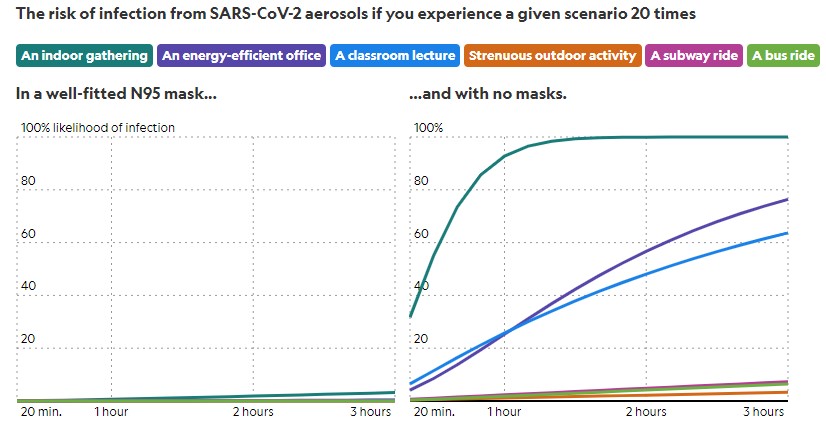
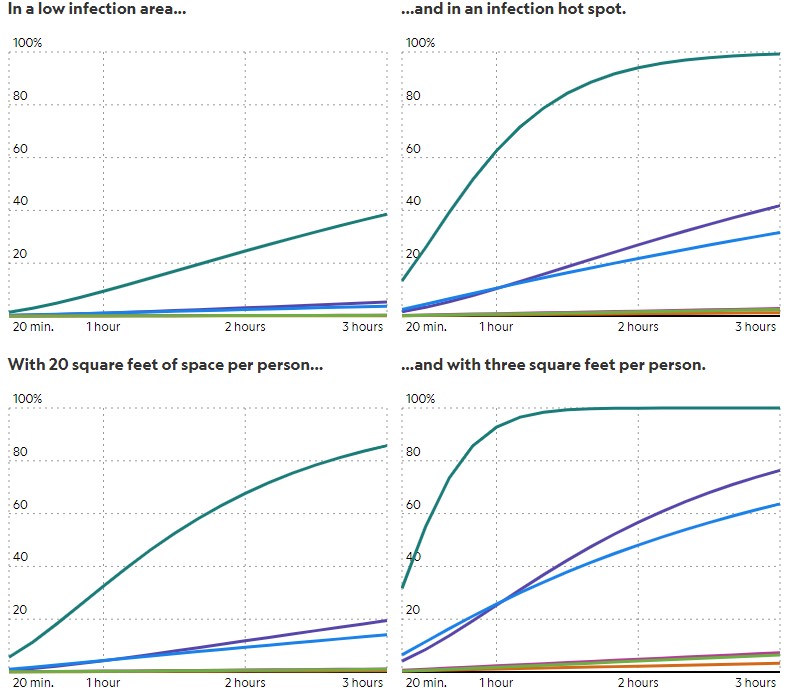
Note: This scenario assumes a well-fitted N95 mask blocks 95 percent of airborne particles. A hot spot is defined as having an infection rate of 3 percent in the local population, and a low infection area has a 0.03 percent infection rate. Unless otherwise specified, the scenarios assume 50 percent of particles pass through masks, 12 square feet of space per person at each event, and an infection rate of 2 percent. The model does not fully account for how your risk increases the closer you get to an infected person, where the concentration of both aerosols and respiratory droplets will be higher. Potential risk from contaminated surfaces is also not included. All scenarios assume constant values for room temperature, pressure, humidity, and how quickly particles settle out of the air onto surfaces due to gravity. The model also assumes that no one in the local population is immune.
The model provides a rough estimation of risk, Jimenez cautions. As with any model, the calculations must make some assumptions, such as requiring the air to be mixed, so the virus is dispersed throughout the room. Still, it can provide valuable clues to the relative risks of different activities.
To calculate the possible aerosol risks in various environments, users can tweak a host of parameters, such as the size of a group, the room size, or the effectiveness of masks.
The risk also depends on the prevalence of the disease in your area, which users can input into the model to change the potential number of infected people in a given group.
An important note: the model does not account for how the risk increases with closer proximity, where droplet and aerosol concentrations will be higher, or for people touching their eyes or noses with contaminated hands.
The model underscores the importance of widespread use of masks and the risks of COVID-19 transmission in crowded rooms and poorly ventilated conditions—and in any of these settings, time is key, says Linsey Marr, a civil and environmental engineer at Virginia Tech who specializes in airborne transmission of viruses and provided feedback on the model. The longer anyone spends in a poorly ventilated or crowded space, the greater the predicted risk of falling ill.
Measure your own risk here.




